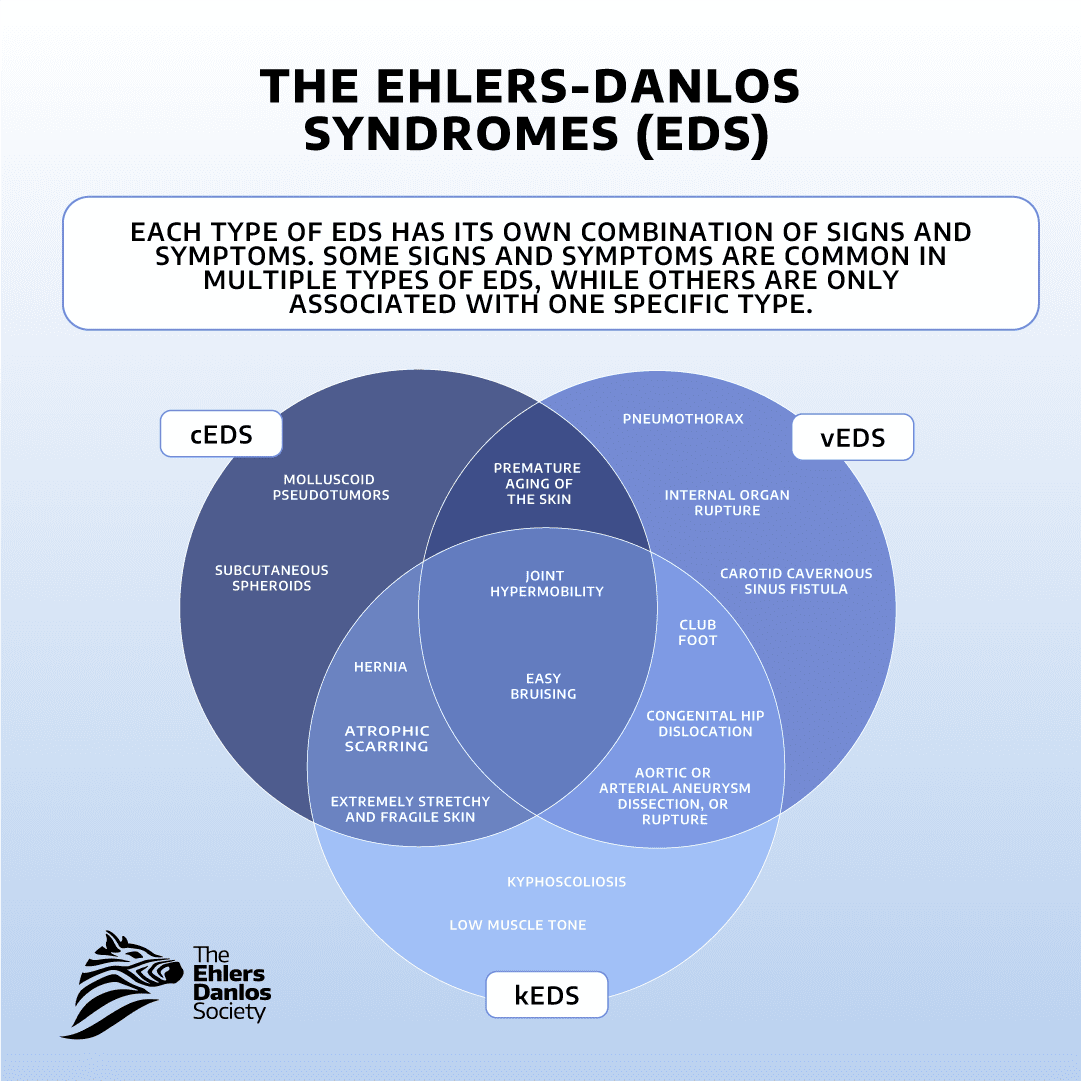
The Ehlers-Danlos syndromes (EDS) are a group of 13 heritable connective tissue disorders. The conditions are caused by genetic changes that affect connective tissue. Each type of EDS has its own set of features with distinct diagnostic criteria. Some features are seen across all types of EDS, including joint hypermobility, skin hyperextensibility, and tissue fragility.
What is EDS?
What is joint hypermobility?
Joint hypermobility means that a person’s joints have a greater range of motion than is expected or usual. Some people have joint hypermobility that does not cause them pain or other issues. However, some people with joint hypermobility also have joint instability. Joint instability occurs when the bones of a joint aren’t held in place securely. This can lead to joint subluxations, dislocations, sprains, and other injuries. Joint instability can cause both acute and chronic pain and interfere with daily life.
Joint hypermobility is observed throughout the body in most types of EDS, but hypermobility may be limited to the hands and feet in some types. Although joint hypermobility is observed across all types of EDS, not everyone with a type of EDS has joint hypermobility. You can read more about joint hypermobility here.
What is skin hyperextensibility?
Skin hyperextensibility means that the skin can be stretched beyond the normal range. Skin extensibility, or skin stretchiness, is measured by pinching and lifting the skin on the volar surface (same side as the palm of the hand) at the middle of the non-dominant forearm. Skin is hyperextensible if it stretches greater than 1.5 cm. Mild skin hyperextensibility may be observed in people with any type of EDS. More severe skin hyperextensibility, greater than 2 cm, is observed in certain types of EDS.
People with a type of EDS may also have other skin characteristics and symptoms, such as unusual skin texture, skin fragility, very thin skin, delayed wound healing, and abnormal scarring. Not everyone with a type of EDS has skin hyperextensibility or unusual skin characteristics.
What is tissue fragility?
Tissue fragility means that the body’s organs and other structures are more vulnerable to damage. Tissue fragility can present as easy bruising and poor wound healing in many types of EDS. Some types of EDS can also cause severe fragility of the skin, blood vessels, abdominal organs, eyes, gums, and bones.
What are the types of EDS?
The current classification includes 13 types of Ehlers-Danlos syndrome. Each type has its own genetic causes. This results in a unique set of features for each type of EDS.
-
Hypermobile EDS (hEDS) »
- Approximate Prevalence
- 1 in 3,100 – 5,000
- Associated Gene(s) and Affected Protein(s)
- Unknown (Unknown)
- Inheritance Pattern
- Autosomal Dominant
- Distinguishing Features
- Generalized joint hypermobility
Joint instability
Chronic pain
-
Classical EDS (cEDS) »
- Approximate Prevalence
- 1 in 20,000 – 40,000
- Associated Gene(s) and Affected Protein(s)
- COL5A1 (Type V collagen)
COL5A2 (Type V collagen)
COL1A1 (Type I collagen) - Inheritance Pattern
- Autosomal Dominant
- Distinguishing Features
- Skin fragility with extensive atrophic scarring
Very stretchy skin with velvety or doughy texture
-
Vascular EDS (vEDS) »
- Approximate Prevalence
- 1 in 100,000 – 200,000
- Associated Gene(s) and Affected Protein(s)
- COL3A1 (Type III collagen)
COL1A1(Type I collagen) - Inheritance Pattern
- Autosomal Dominant
- Distinguishing Features
- Arterial fragility with aneurysm/dissection/rupture
Organ fragility and rupture
Pneumothorax
-
Periodontal EDS (pEDS) »
- Approximate Prevalence
- Less than 1 in 1,000,000
- Associated Gene(s) and Affected Protein(s)
- C1R (C1r)
C1S (C1s) - Inheritance Pattern
- Autosomal Dominant
- Distinguishing Features
- Severe, early-onset gum disease with tooth loss
Pretibial plaques (discoloration of shins)
-
Kyphoscoliotic EDS (kEDS) »
- Approximate Prevalence
- Less than 1 in 1,000,000
- Associated Gene(s) and Affected Protein(s)
- PLOD1 (LH1)
FKBP14 (FKBP22) - Inheritance Pattern
- Autosomal Recessive
- Distinguishing Features
- Congenital/early-onset kyphoscoliosis
Congenital hypotonia
-
Spondylodysplastic EDS (spEDS) »
- Approximate Prevalence
- Less than 1 in 1,000,000
- Associated Gene(s) and Affected Protein(s)
- B4GALT7 (β4GalT7)
B3GALT6 (β3GalT6)
SLC39A13 (ZIP13) - Inheritance Pattern
- Autosomal Recessive
- Distinguishing Features
- Short stature
Muscle weakness
Limb bowing
Craniofacial features
-
Brittle cornea syndrome (BCS) »
- Approximate Prevalence
- Less than 1 in 1,000,000
- Associated Gene(s) and Affected Protein(s)
- ZNF469 (ZNF469)
PRDM5 (PRDM5) - Inheritance Pattern
- Autosomal Recessive
- Distinguishing Features
- Severe problems with the cornea of the eye
Hearing loss
-
Arthrochalasia EDS (aEDS) »
- Approximate Prevalence
- Less than 1 in 1,000,000
- Associated Gene(s) and Affected Protein(s)
- COL1A1 (Type I collagen)
COL1A2 (Type I collagen) - Inheritance Pattern
- Autosomal Dominant
- Distinguishing Features
- Severe joint hypermobility
Congenital bilateral hip dislocation
-
Musculocontractural EDS (mcEDS) »
- Approximate Prevalence
- Less than 1 in 1,000,000
- Associated Gene(s) and Affected Protein(s)
- CHST14 (D4ST1)
DSE (DSE) - Inheritance Pattern
- Autosomal Recessive
- Distinguishing Features
- Congenital multiple contractures
Craniofacial features
-
Classical-like EDS (clEDS) »
- Approximate Prevalence
- Less than 1 in 1,000,000
- Associated Gene(s) and Affected Protein(s)
- TNXB (Tenascin XB)
- Inheritance Pattern
- Autosomal Recessive
- Distinguishing Features
- Stretchy, velvety skin without atrophic scarring
Foot deformities
Leg swelling
-
Dermatosparaxis EDS (dEDS) »
- Approximate Prevalence
- Less than 1 in 1,000,000
- Associated Gene(s) and Affected Protein(s)
- ADAMTS2 (ADAMTS-2)
- Interitance Pattern
- Autosomal Recessive
- Distinguishing Features
- Extreme skin fragility
Craniofacial features
Loose, excessive skin
Severe bruising
Short limbs
-
Myopathic EDS (mEDS) »
- Approximate Prevalence
- Less than 1 in 1,000,000
- Associated Gene(s) and Affected Protein(s)
- COL12A1 (Type XII collagen)
- Inheritance Pattern
- Autosomal Dominant or Recessive
- Distinguishing Features
- Congenital hypotonia
Proximal joint contractures
-
Cardiac-valvular EDS (cvEDS) »
- Approximate Prevalence
- Less than 1 in 1,000,000
- Associated Gene(s) and Affected Protein(s)
- COL12A2 (Type I collagen)
- Inheritance Pattern
- Autosomal Recessive
- Distinguishing Features
- Severe heart valve insufficiency
| Type of EDS
(In order of estimated prevalence) |
Approximate Prevalence | Associated Gene(s) | Affected Protein(s) | Inheritance Pattern |
Distinguishing Features |
| 1 in 3,100 – 5,000 | Unknown | Unknown | Autosomal Dominant |
|
|
| 1 in 20,000 – 40,000 | COL5A1 | Type V collagen | Autosomal Dominant |
|
|
| COL5A2 | Type V collagen | ||||
| COL1A1 | Type I collagen | ||||
| 1 in 100,000 – 200,000 | COL3A1 | Type III collagen | Autosomal Dominant |
|
|
| COL1A1 | Type I collagen | ||||
| Less than 1 in 1,000,000 | C1R | C1r | Autosomal Dominant |
|
|
| C1S | C1s | ||||
| Less than 1 in 1,000,000 | PLOD1 | LH1 | Autosomal Recessive |
|
|
| FKBP14 | FKBP22 | ||||
| Less than 1 in 1,000,000 | B4GALT7 | β4GalT7 | Autosomal Recessive |
|
|
| B3GALT6 | β3GalT6 | ||||
| SLC39A13 | ZIP13 | ||||
| Less than 1 in 1,000,000 | ZNF469 | ZNF469 | Autosomal Recessive |
|
|
| PRDM5 | PRDM5 | ||||
| Less than 1 in 1,000,000 | COL1A1 | Type I collagen | Autosomal Dominant |
|
|
| COL1A2 | Type 1 collagen | ||||
| Less than 1 in 1,000,000 | CHST14 | D4ST1 | Autosomal Recessive |
|
|
| DSE | DSE | ||||
| Less than 1 in 1,000,000 | TNXB | Tenascin XB | Autosomal Recessive |
|
|
| Less than 1 in 1,000,000 | ADAMTS2 | ADAMTS-2 | Autosomal Recessive |
|
|
| Less than 1 in 1,000,000 | COL12A1 | Type XII collagen | Autosomal Dominant or Recessive |
|
|
| Less than 1 in 1,000,000 | COL1A2 | Type I collagen | Autosomal Recessive |
|
Frequently Asked Questions
How common is EDS?
Each type of EDS has a different prevalence in the population. Hypermobile EDS (hEDS) is the most common type of EDS by far. hEDS accounts for about 90% of EDS cases and is thought to affect at least 1 in 3,100-5,000 people. hEDS is currently classified as a rare disorder, but the true prevalence is not known and may be underestimated. Classical EDS (cEDS) and vascular EDS (vEDS) are much rarer than hEDS. cEDS affects roughly 1 in 20,000-40,000 people. vEDS affects about 1 in 100,000-200,000 people. All other types of EDS are classified as ultra-rare, affecting less than 1 in 1 million people. Several types of EDS have only been reported in a few affected families.
You can read more about the prevalence of EDS here.
What causes EDS?
Each type of EDS is caused by variants in specific genes that provide the instructions for making collagens and related proteins. Some types of EDS are associated with multiple different genes. The genetic cause(s) of hEDS have not been identified.
What are connective tissue and collagen?
Connective tissue is found throughout the body, where it provides support, protection, and structure to other parts of the body. Connective tissue disorders are caused by issues that prevent connective tissue from functioning properly.
Collagen is the primary component of connective tissue. There are different types of collagens with different functions. The Ehlers-Danlos syndromes are caused by changes in the genes that affect the structure and function of collagen and related connective tissue proteins.
Can EDS be inherited?
The Ehlers-Danlos syndromes can be passed on from parent to child. Each type of EDS is inherited in either a dominant or recessive inheritance pattern.
A dominant inheritance pattern means that just one copy of a genetic variant (passed down from one parent) is needed to inherit the condition. If a person has a condition with a dominant inheritance pattern, each of their children will have a 50% chance of inheriting the condition. A recessive inheritance pattern means that a person must inherit two copies of the genetic variant (one from each parent) in order to have the condition.
Although the genetic cause(s) of hEDS are not yet known, family histories suggest this condition has a dominant inheritance pattern.
A person may be the first one in their family to have a type of EDS. This is called a de novo mutation. You can read more about the inheritance of EDS here.
What are the signs and symptoms of EDS?
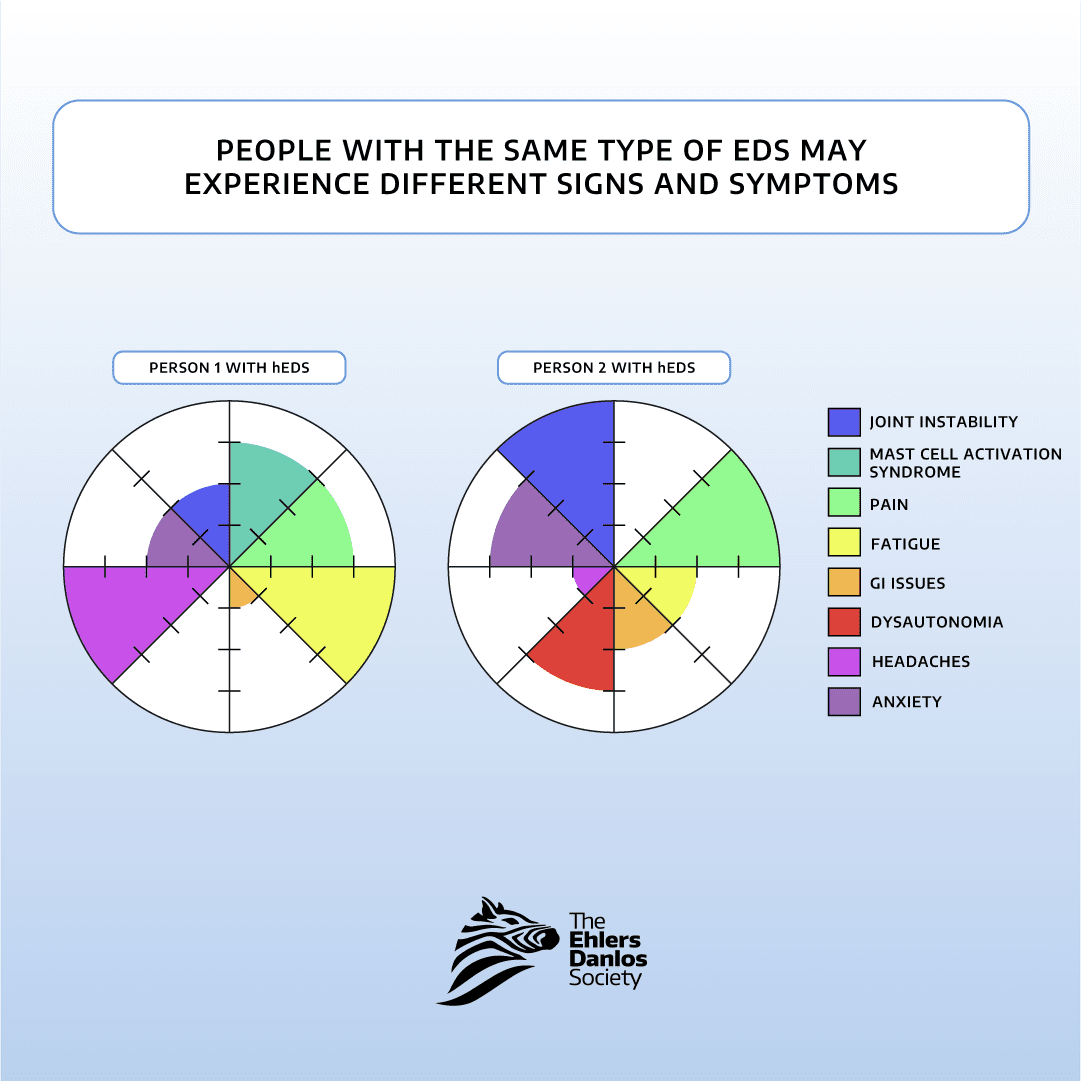
Each type of EDS is associated with different symptoms and characteristics. Some symptoms are common across all types of EDS, such as joint hypermobility, pain, and fatigue. Other symptoms are only observed in specific types of EDS. Even within the same type of EDS, people can experience very different symptoms from each other.
There are also many other medical conditions that are often seen in people with EDS. These include types of dysautonomia and mast cell diseases. These are often called comorbidities or comorbid conditions.
How is EDS diagnosed?
Each type of EDS has its own clinical diagnostic criteria. Clinical diagnostic criteria are a set of symptoms and characteristics observed in each condition. If a person meets the diagnostic criteria for a type of EDS, a genetic test should be done to confirm the diagnosis.
The genetic cause(s) of hEDS have not yet been identified, so there is currently no genetic test available to diagnose hEDS. The diagnosis of hEDS is given to those who meet the clinical diagnostic criteria for hEDS.
If a person has symptomatic joint hypermobility but does not meet the diagnostic criteria for any type of EDS or other condition that can cause similar symptoms, then the hypermobility spectrum disorders (HSD) should be considered. You can read more about HSD here.
How is EDS managed?
There are no disease-specific treatments for any type of EDS, so EDS is managed by addressing each person’s symptoms. The Ehlers-Danlos syndromes can cause a variety of symptoms in different areas of the body. Therefore, people with a type of EDS often require multiple providers in different specialties to manage their care. Even within the same type of EDS, two people may have very different symptoms and respond differently to different management strategies. Each person should work with their care team to develop a care plan that meets their individual needs.
How were the Ehlers-Danlos syndromes named?
The Ehlers-Danlos syndromes (EDS) are named after two doctors, Dr. Edvard Lauritz Ehlers and Dr. Henri-Alexandre Danlos, who described the condition in the early twentieth century.
The classification of the types of Ehlers-Danlos syndrome has changed over time as these conditions were better understood. In 1986, the Berlin classification introduced 11 types of EDS, each designated by a Roman numeral. In 1998, the Villefranche classification was established based on an updated understanding of the types of EDS and their genetic causes. It included 6 types of EDS and replaced the Roman numeral system with descriptive names for each type. Major and minor criteria were also established for each type of EDS.
In 2017, The International Consortium on EDS and HSD published the 2017 international classification of the Ehlers-Danlos syndromes. This current classification includes 13 types of EDS. Each type of EDS has a descriptive name which is abbreviated using a lowercase letter to differentiate between the types of EDS. For example, hypermobile Ehlers-Danlos syndrome is abbreviated to hEDS. The different types of EDS are no longer described using numbers or Roman numerals; the terms EDS type 3 and EDS type III are no longer used.
The 2017 classification also introduced the hypermobility spectrum disorders (HSD). As of 2017, joint hypermobility syndrome (JHS) and benign joint hypermobility syndrome (BJHS) are outdated terms that should no longer be used when making a diagnosis. Most people who were previously diagnosed with joint hypermobility syndrome or a similar diagnosis are now classified as having either hEDS or a type of HSD. If someone was diagnosed with hEDS before the 2017 criteria, there is no reason to seek a new diagnosis unless they decide to participate in research or need to be reassessed for some other reason.
Since the 2017 classification, researchers have identified additional genetic variants that cause symptoms similar to those seen in the Ehlers-Danlos syndromes. These variants may represent new types of EDS or may fall under one of the current types of EDS.
Learn more about the AEBP1 variants here.
Learn more about the COL1A1/COL1A2 variants here.
The classification of EDS and HSD will continue to evolve as we learn more about these conditions through research.
